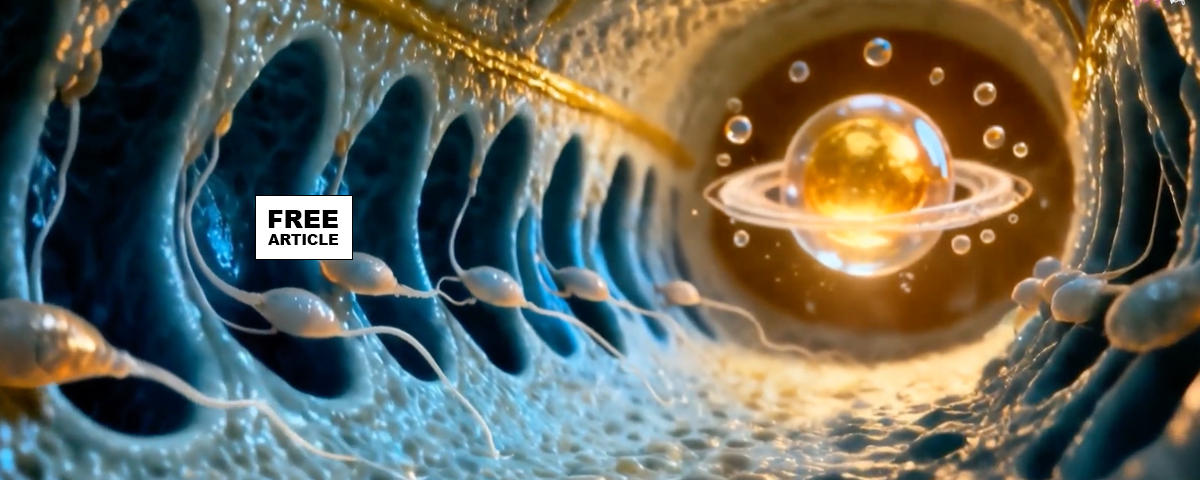
The timing of sexual intercourse in relation to ovulation strongly influences the chance of conception. In the days leading up to ovulation, rising estrogen levels cause the cervix to produce thin, watery, and highly permeable mucus that facilitates sperm passage, creating an optimal environment for fertilization. During ovulation, progesterone plays a crucial role in transforming cervical mucus from a receptive, fertile state to a less hospitable one. After ovulation, progesterone levels increase sharply, inducing a physiological change in the cervical mucus. Progesterone causes the cervical mucus to become thick, viscous, and scant, primarily due to increased secretion of glycoproteins and dehydration of the mucus. The resulting high-viscosity mucus acts as a physical barrier, preventing sperm from entering the uterus and protecting the reproductive tract from pathogens. This transformation under the influence of progesterone effectively marks the end of the fertile window, playing a vital role in preventing conception. The cyclical modulation of cervical mucus by progesterone is a key physiological mechanism to regulate fertility, ensuring that sperm can only traverse the cervix during the optimal fertile period.
The survival time of sperm within the female reproductive tract varies depending on their location. In the cervical crevices and crypts, sperm can survive for approximately 24 to 48 hours, as this environment provides a protective niche that shields sperm from the acidic vaginal pH and immune responses, allowing them to remain viable while awaiting ovulation. Once sperm enter the fallopian tubes, their lifespan can extend up to 72 hours or more, especially if the environment remains optimal for motility and fertilization. The ovum, on the other hand, has a much shorter viability window, typically around 12 to 24 hours after ovulation, during which fertilization must occur for pregnancy to be successful. The role of retrograde cervical contractions is crucial in sperm transport; these rhythmic muscle contractions help propel sperm from the cervix into the upper reproductive tract, facilitating their movement through the cervical canal and into the fallopian tubes where they await the egg. These contractions coordinate with hormonal signals—particularly rising levels of estrogen—to optimize the timing during ovulation, ensuring that sperm reach the ovum efficiently. This intricate interplay between sperm survival, cervical physiology, and uterine contractions ensures the best chances for fertilization to occur.
To ensure conception, sperm should be present in the female reproductive tract in the days leading up to ovulation. As noted, sperm can survive for approximately 3 to 5 days within the cervical crevices and the female reproductive tract due to the protective and nourishing environment, particularly when the cervical mucus is fertile and estrogen-rich. This mucus is thin and alkaline, facilitating sperm viability and motility, which allows sperm to traverse from the cervix into the uterus and fallopian tubes. Therefore, intercourse occurring up to five days before ovulation can still result in conception, as viable sperm will be present when the ovum is released. Given that the ovum has a short viability span of about 12 to 24 hours post-ovulation, having sperm already present in the fallopian tubes maximizes the chances of fertilization as soon as ovulation occurs. This timing underscores the importance of the fertile window, which is typically the five days preceding ovulation and the day of ovulation itself: “the optimal period for achieving conception”.
Among healthy women trying to conceive, nearly all pregnancies can be attributed to intercourse during a five-day period ending on the day of ovulation.