Inverse vaccines represent one of the most innovative emerging strategies in autoimmune disease, especially relevant for women, who are disproportionately affected by conditions like Systemic Lupus Erythematosus, Rheumatoid Arthritis, and Multiple Sclerosis. Unlike traditional vaccines, which stimulate the immune system to recognize and attack foreign pathogens, inverse vaccines are designed to do the opposite: they selectively retrain the immune system to tolerate the body’s own tissues by targeting the specific autoantigens that trigger disease. Mechanistically, these therapies exploit the biology of immune tolerance by delivering disease-associated antigens in a context that promotes immune “silencing” rather than activation, often by engaging tolerogenic antigen-presenting cells such as dendritic cells. This process encourages the expansion of regulatory T cells and the suppression or deletion of autoreactive T cells, effectively turning off the pathological immune response without broadly compromising immune defenses. Early clinical studies, particularly in conditions like Celiac Disease and Type 1 Diabetes, have demonstrated that inverse vaccines can reduce inflammatory responses and preserve tissue function with a high degree of specificity.
Inverse vaccines are designed to selectively suppress harmful immune responses rather than stimulate them, making them especially promising for treating autoimmune diseases such as multiple sclerosis or type 1 diabetes. Their mechanism of action centers on inducing immune tolerance to specific self-antigens. Typically, these vaccines deliver disease-relevant antigens in a context that does not activate inflammation, for example, by coupling the antigen to nanoparticles, apoptotic cells, or tolerogenic carriers. These formulations are preferentially taken up by antigen-presenting cells like dendritic cells in a non-inflammatory state, which then present the antigen to T cells without the necessary co-stimulatory signals. As a result, autoreactive T cells are either deleted (clonal deletion), rendered inactive (anergy), or converted into regulatory T cells that actively suppress immune responses. This process mimics natural peripheral tolerance mechanisms and reduces pathological immune activity without broadly compromising the entire immune system, distinguishing inverse vaccines from traditional immunosuppressive therapies.
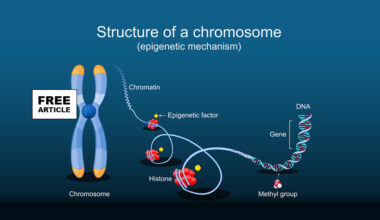
In women, the implications are especially significant because autoimmune diseases are often driven by complex interactions between hormonal fluctuations, X chromosome–linked immune regulation, and heightened immune reactivity. Inverse vaccines offer a way to precisely interrupt these disease-specific immune pathways without interfering with normal immune surveillance, which is particularly important given women’s higher baseline immune responsiveness. Additionally, these therapies may be tailored to different stages of a woman’s life, such as postpartum immune shifts or perimenopausal transitions, when autoimmune diseases often flare or emerge. Another key advantage is the potential to intervene early in the disease process, or even in high-risk individuals identified through genetic or biomarker screening, thereby preventing irreversible tissue damage. While still largely in experimental and early clinical phases, inverse vaccines are widely viewed as a potential “functional cure” approach, shifting the paradigm from chronic immunosuppression to precise immune re-education, with the promise of long-term remission and fewer systemic side effects.