Infertility is defined by the American College of Obstetricians and Gynecologists as the inability to become pregnant after 12 months or more of unprotected intercourse for women under 35 and after six months for women over 35.
Infertility in women can stem from a variety of root causes, often involving complex interactions between hormonal, structural, and physiological factors. Hormonal imbalances are a common culprit, with conditions like polycystic ovary syndrome (PCOS) leading to irregular ovulation due to excess androgen production. Thyroid disorders, such as hypothyroidism or hyperthyroidism, can also disrupt menstrual cycles and affect ovulation. Structural abnormalities, including blocked or damaged fallopian tubes, often result from pelvic inflammatory disease or endometriosis, affecting the egg’s ability to meet sperm or implant in the uterus. Uterine issues, such as fibroids or polyps, can interfere with implantation or cause miscarriages. Age-related decline in ovarian reserve significantly impacts fertility, as the quantity and quality of eggs diminish over time, especially after age 35. Lifestyle factors like obesity, excessive alcohol consumption, smoking, and high stress levels further exacerbate infertility by affecting hormonal balance and overall reproductive health. In some cases, genetic factors or autoimmune disorders may also play a role, complicating the diagnosis and treatment. Comprehensive evaluation, including hormonal assessments, imaging studies, and lifestyle analysis, is crucial to identifying and addressing the specific causes of infertility, paving the way for effective management and potential conception.
Common Causes of Infertility.
- Fallopian Tube Abnormalities Are Present In 25% – 35% OF All Infertile Women.
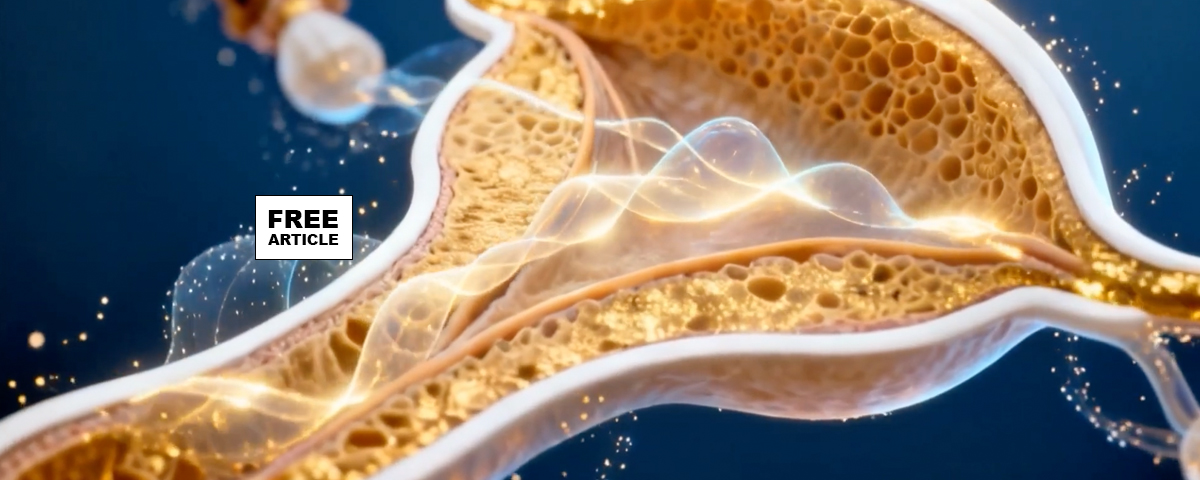
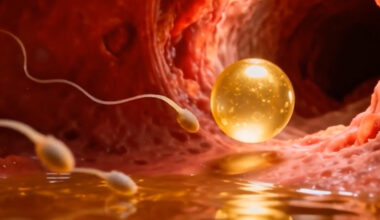
After traversing the cervix and reaching the fallopian tube sperm can fertilize an egg. Fertilization is the process by which male and female gametes fuse to form a zygote (a unicellular structure with a complete set of 46 chromosomes). Fertilization usually takes place in the ampulla, the widest part of the fallopian tube, within 12 to 24 hours after ovulation.
Tubal blockage resulting from endometriosis, inflammation or infection, negatively influences tubal function. Tubal dysfunction may also occur in the presence of unobstructed fallopian tubes, as in the case of acquired or congenital disorders of ciliary function or abnormal tubal peristalsis, contributing to infertility or ectopic pregnancy. As a result, identifying both tubal pathology and tubal patency has been traditionally a cornerstone of the workup of an infertile couple. Due to their small size, the fallopian tubes are easily damaged or blocked. The fallopian tubes are often blocked or damaged because of scarring on the walls of the tubes caused by infection. Aside from infection, which can be due to various causes, tubes may be blocked by endometriosis or damaged from surgery. The more frequent causes of tubal occlusion follow:
Endometriosis is when tissue from a woman’s endometrium, the lining of the uterus, begins to grow outside of the uterus on other pelvic organs. During menstruation the endometrium is typically shed and released from a woman’s body as flow from her period. However, the endometrial tissue that is growing outside of the uterus does not shed like normal tissue. This causes inflammation and can lead to the development of scar tissue in the fallopian tube.
Pelvic inflammatory disease (PID) is an infection that can develop when sexually transmitted diseases (STDs) or other infections go untreated. It is typically caused by gonorrhea or chlamydia. PID causes inflammation near the fallopian tubes, which can lead to the development of scar tissue and blockages.
Past surgeries can also be a cause of damaged or blocked fallopian tubes. In particular, surgery for medical problems like uterine fibroids or endometriosis and other types of abdominal surgery may cause scarring that affects an egg’s ability to travel through the fallopian tubes.
Ectopic pregnancy is when a fertilized egg implants in the fallopian tubes, rather than in the uterus. Because fallopian tubes are small and narrow, the fertilized egg does not have the room it needs to grow. This can cause the fallopian tubes to rupture, which is life threatening and can render a woman infertile.
If a doctor identifies an ectopic pregnancy before the fallopian tube ruptures, then surgery can be performed to remove the fertilized egg. This surgery can often lead to fallopian tube scarring and sometimes removal
- Abnormal uterine contractions even in mild endometriosis can lead to Infertility.
Abnormal Uterine contraction in Endometriosis is responsible for pain and infertility. The inner myometrium, the uterine muscle, is responsible for peristaltic-like, wavelike movements in the non-pregnant uterus. Hyperperistalsis and dysperistalsis (abnormal) of the uterus underlie many important disorders such as dysmenorrhea (painful menses) infertility, implantation failure and preterm birth.
The main function of the inner myometrium appears to be the modulation of uterine peristalsis, an area that increasingly is believed to play a significant role in fertility. Inner myometrial contractions vary in orientation, amplitude, and frequency throughout the menstrual cycle, under the influence of the sex hormones, estradiol and progesterone. Studies have shown that, in the follicular phase (early phase) of the cycle when the ovaries produce mature follicles which contain eggs, contractions are predominantly cervico-fundal (from the bottom of the uterus the cervix toward the top, specifically the fallopian tubes), and their amplitude and frequency increase significantly as ovulation approaches. There is evidence that this facilitates sperm ascension towards the distal (far) end of the fallopian tubes, where fertilization takes place. After ovulation, the uterus undergoes, under the influence of progesterone, progressive relaxation that culminates during the mid-luteal phase (second half of the menstrual cycle) which may assist proper embryo positioning in the midsection of the uterine cavity and, thus, facilitate embryo implantation while also improving the supply of oxygen and nutrients.
Women suffering from infertility in association with mostly mild endometriosis were subjected to vaginal sonography of uterine peristalsis during the menstrual period, the early, mid- and late follicular phases, and the mid-luteal phase of the menstrual cycle. The data obtained were compared with those of healthy controls. Women with endometriosis displayed a marked uterine hyperperistalsis that differed significantly from the peristalsis of the women without endometriosis (controls) during the early and mid- follicular and mid-luteal phases. During the late follicular phase of the cycle, uterine peristalsis in women with endometriosis became dysperistaltic (abnormal), arrhythmic and convulsive in character, while in controls, peristalsis continued to show long and regular cervico-fundal (normal) contractions.
This uterine dysperistalsis even in mild endometriosis, underlies many important disorders such as dysmenorrhea (pain), retrograde menses, and infertility due to interference with normal sperm transport.
- Polycystic Ovary Syndrome
Infertility related to polycystic ovary syndrome (PCOS) is primarily due to hormonal imbalances that disrupt normal ovulation. PCOS is characterized by elevated levels of androgens, which can hinder the development and release of mature eggs from the ovaries, leading to irregular or absent menstrual cycles. This anovulation is the main cause of infertility in women with PCOS. Additionally, insulin resistance, a common feature of PCOS, exacerbates hormonal disturbances by increasing insulin levels, which in turn stimulate the ovaries to produce more androgens. This cycle further impedes ovulation and contributes to symptoms like hirsutism and acne. The hormonal imbalance also affects the endometrial lining, making it less receptive to implantation even if fertilization occurs. Over time, the chronic lack of regular ovulation can lead to the formation of multiple ovarian cysts, which worsen hormonal disruptions. Lifestyle factors such as obesity can intensify the metabolic and reproductive symptoms, requiring weight management as part of the therapeutic approach.