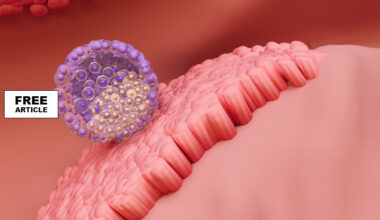
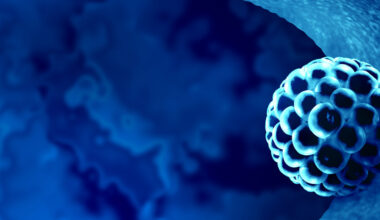
Breastfeeding plays a foundational role in shaping the infant microbiome during a narrow and highly influential developmental window. Human milk is not simply nutrition; it is a biologically active fluid containing complex sugars called human milk oligosaccharides (HMOs), immunoglobulins such as secretory IgA, antimicrobial peptides, cytokines, growth factors, and even live immune cells. HMOs are particularly important because they are indigestible by the infant but selectively feed specific beneficial bacteria, most notably Bifidobacterium species, helping them dominate the early gut ecosystem. This selective feeding creates a microbiome rich in bacteria that produce short-chain fatty acids, lower gut pH, strengthen the intestinal barrier, and suppress the growth of potentially pathogenic organisms. In essence, breast milk functions as a biological “architect,” directing which microbes thrive and which do not.
This early microbial patterning has systemic consequences. The infant immune system is immature at birth and must learn to distinguish harmless stimuli from dangerous pathogens. A breastmilk-shaped microbiome helps calibrate immune tolerance by promoting regulatory T cell development and balanced inflammatory responses. Secretory IgA in milk coats the infant gut lining, limiting bacterial translocation while still allowing immune education to occur. Over time, this coordinated interaction between milk components, microbes, and the developing immune system reduces the risk of infections in infancy and is associated with lower rates of allergic disease, eczema, and asthma later in childhood. Emerging research also suggests that breastfeeding duration influences microbial development not only in the gut but in the respiratory tract, which may partially explain observed reductions in respiratory illness and wheezing disorders.
Beyond immunity, microbiome programming may influence metabolic and neurodevelopmental outcomes. Gut bacteria help regulate energy extraction, insulin sensitivity, and fat storage through metabolic signaling pathways. A microbiome enriched in beneficial bifidobacteria and butyrate-producing organisms appears to support healthier weight trajectories in childhood. Additionally, microbial metabolites interact with the gut-brain axis, influencing neurotransmitter production, stress responses, and brain maturation. While causality is still being clarified, longitudinal cohort studies link longer breastfeeding duration with favorable cognitive and behavioral outcomes, possibly mediated in part by microbiome-dependent mechanisms.
Timing matters. The first three to six months represent a critical ecological window during which feeding patterns exert outsized influence. Early supplementation or early weaning can shift microbial composition toward more adult-like, diverse, but not necessarily developmentally optimized, patterns. Although diversity is generally considered beneficial in adults, in early infancy a bifidobacteria-dominant, breastmilk-adapted microbiome appears protective. As solid foods are introduced, the microbiome gradually transitions, but the foundational immune and metabolic programming established during exclusive breastfeeding may have durable effects.
Importantly, breastfeeding is one of several factors shaping microbial development. Mode of delivery, antibiotic exposure, maternal health, environment, and genetics also play significant roles. However, breastfeeding uniquely provides both the microbes’ preferred substrates and immune regulators that coordinate microbial colonization with immune maturation. For this reason, it is increasingly viewed not just as feeding, but as a form of biological signaling that programs long-term health trajectories through microbiome-mediated pathways.